Suggested reading
|
Bridget's stories

Back in the early to mid-70s when I was pushing the boundaries, there was a fair bit of media attention about how young people were ‘experimenting’ with drugs. My friends and I were incensed. We didn’t experiment with drugs. We knew exactly what we were doing. Read more here
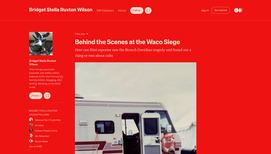
I like an adventure. So when the siege at Waco, Texas, was happening in 1993 it seemed like a good idea to fly from Auckland New Zealand to cover it as a freelance reporter.
I’d been interested in cults for a while and the Branch Davidian compound at Mt Carmel near Waco housed a particularly interesting one. Read more here |

Esteemed Study Identifies Sexual Addiction as Identifiable and Diagnosable
By Robert Weiss LCSW, CSAT-S
All Highly Pleasurable Substances and Behaviors Have Addiction Potential
Led by Dr. Valerie Voon (pictured right), a group of researchers at the University of Cambridge (UK) recently published a detailed fMRI study showing that the brain activity in sex addicts, when they are shown pornography, mirrors the brain activity in drug addicts when they are exposed to drug-related imagery. This study strongly suggests that sexual addiction not only exists, but in fact manifests in profoundly similar ways to other more readily accepted forms of addiction like alcoholism, drug addiction, and Internet addiction.
What the Research Measured
Dr. Voon’s team recruited 19 heterosexual male sex addicts and 19 similarly aged non-sex addicted heterosexual males. For all subjects, exclusionary criteria included being under 18, a history of substance abuse/addiction, being a current user of illicit substances (including marijuana), and having a serious psychiatric disorder like depression, OCD, bipolar disorder, etc. All participants in the study were asked to view video clips from one of five categories: explicit sexual imagery (consensual sex between men and women), erotic imagery (dressed women dancing, brushing their thigh, etc.), non-sexual exciting imagery (skiing, skydiving, etc.), monetary imagery (coins and bills changing hands, scattered, etc.), and neutral imagery (various landscapes).
While viewing the videos, subjects’ brain activity was monitored using fMRI imaging, allowing researchers to track which brain regions were activated by which videos. The idea was to see if the brain response of sex addicts differs from the brain response of non-sex addicts, and also to see if the brain response of sex addicts is similar to the brain response of drug addicts. (For this last part, researchers compared the results of this study to the results of fMRI studies focused on drug addiction.)
Researchers also asked the participants to answer, in regard to each video:
- How much did this video increase your sexual desire?
- How much did you like this video?
Findings and Conclusions
Basic findings from the initial interview portion of the research found that sex addicted subjects first viewed online sexually explicit material at an earlier age, had greater Internet use in general, and spent a much larger percentage of their time online viewing sexually explicit material (25.49% compared to 4.49%). These findings mesh with existing research of compulsive sexual activity, and they are certainly no surprise to clinicians who treat sexual addiction. The “younger age of first use” is particularly notable, as substance addiction research has also shown a consistent link between age of first use and propensity for addiction later in life.
The fMRI results, of course, are of much greater significance. The researchers found that when viewing sexual imagery three significant brain regions – the ventral striatum (processing rewards), the dorsal anterior cingulate (anticipating rewards), and the amygdala (processing the significance of events and emotions) – were activated in sex addicts to a much greater degree than in non-sex addicts. Furthermore, these three regions are similarly activated in drug addicts when they are exposed to drug-related imagery. In other words, the brains of sex addicts respond to sexual stimuli differently than the brains of non-sex addicts, and, just as importantly, the brains of sex addicts respond to sexual stimuli in the same way that the brains of drug addicts respond to drug-related stimuli.
As for the desiring versus liking questions: In comparison to non-sex addicts, sex addicts showed higher levels of desire for explicitly sexual imagery but not higher levels of like. (With non-sexual videos the scores of sex addicts and non-sex addicts were indistinguishable.) This means that sex addicts, like drug addicts, desire/crave their addiction more than they like/enjoy their addiction. This is another significant link between sexual addiction and other forms of addiction.
The Importance of This Research
As of now, there are no formalized diagnostic criteria for sexual addiction. A proposed Hypersexual Disorder diagnosis was considered for inclusion in the DSM-5 (published by the American Psychiatric Association last year), but ultimately it was dismissed without explanation. This occurred despite the undeniably increasing incidence of sexual addiction in the US and abroad – an increase nearly always driven by digital technology and the 24/7/365 accessibility of intensely stimulating sexual content and potential partners that it provides. In short, as the relatively anonymous and highly affordable accessibility of digital sexual stimuli has increased, so too has the incidence of sexual addiction. It’s just that simple.
Despite the APA’s inexplicable unwillingness to recognize sexual addiction as an official diagnosis, other organizations, most notably the American Society of Addiction Medicine, have been significantly more forward-thinking. ASAM writes:
Addiction is a primary, chronic disease of brain reward, motivation, memory and related circuitry. Dysfunction in these circuits leads to characteristic biological, psychological, social and spiritual manifestations. This is reflected in an individual pathologically pursuing reward and/or relief by substance use and other behaviors. Addiction is characterized by inability to consistently abstain, impairment in behavioral control, craving, diminished recognition of significant problems with one’s behaviors and interpersonal relationships, and a dysfunctional emotional response.
The recently released Cambridge research discussed above is a significant step toward proof and universal acceptance of ASAM’s stance when it comes to sexual addiction, in that the three brain regions delineated as significant in this research coincide directly with reward, motivation, and memory – the same as with Substance Use Disorder and other forms of “DSM approved” addiction. In fact, Dr. Richard Krueger of Columbia University, who served on the physician committee that considered Hypersexual Disorder (aka, Sexual Addiction) for inclusion in the DSM-5, has called the Cambridge research a seminal study supporting the notion that sexual addiction is indeed an identifiable and diagnosable disorder.
Given this, one must ask: Is this research the single piece of evidence that will finally push the always-slow-to-react APA forward into action? Most likely not. So for now nothing much changes in the day-to-day assessment and treatment of sexual addiction. In truth, knowledgeable and properly trained sex addiction specialists have long understood that the best approach to sexual addiction treatment mirrors the methodologies that have proven effective with drug and alcohol addiction and various forms of trauma work. The fact that we now have proof that the brain response is similar with sex addiction and drug addiction merely bolsters this well-established approach.
Even though the APA is unlikely to “legitimize” sexual addiction any time soon, an official diagnosis is almost certainly on the horizon, as the APA simply can’t ignore the findings of a well-designed and meticulously executed study that undeniably links sexual addiction to other forms of addiction. Eventually, like it or not, the APA will have to recognize and accept the continually mounting evidence supporting sexual addiction as a very real and devastating affliction. So in terms of a sexual addiction diagnosis, the question is no longer if, but when.
Robert Weiss LCSW, CSAT-S is Senior Vice President of Clinical Development with Elements Behavioral Health. A licensed UCLA MSW graduate and personal trainee of Dr. Patrick Carnes, he founded The Sexual Recovery Institute in Los Angeles in 1995. He has developed clinical programs for The Ranch in Nunnelly, Tennessee, Promises Treatment Centers in Malibu, and the aforementioned Sexual Recovery Institute in Los Angeles.He has also provided clinical multi-addiction training and behavioral health program development for the US military and numerous other treatment centers throughout the United States, Europe, and Asia. For more information you can visit his website, www.robertweissmsw.com.